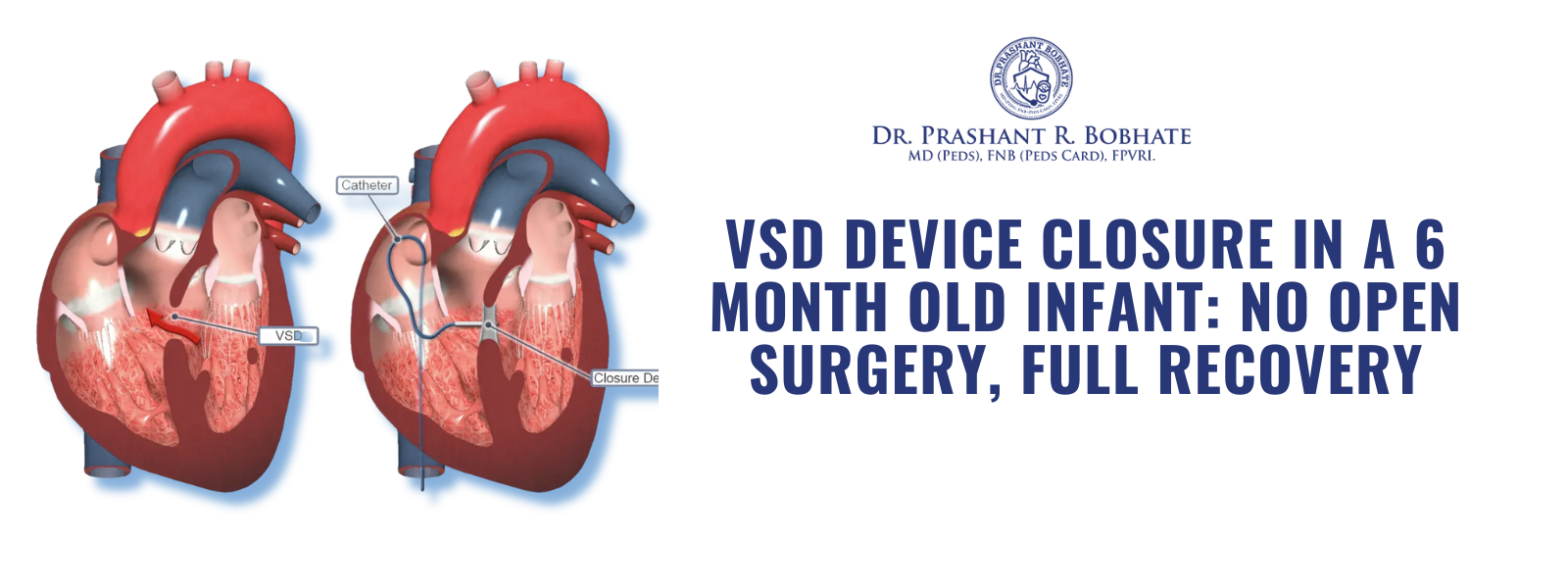
VSD Device Closure in a 6-Month-Old Infant: No Open Surgery, Full Recovery
Patient Profile
Patient Name: Aarav S.
Age: 6 months
Gender: Male
Location: Andheri, Mumbai
Patient Background
Aarav’s mother noticed it before anyone else did. Feeds took too long. He’d drink a little, stop, breathe hard, then try again. Most bottles took over an hour. He wasn’t gaining weight the way he should. Some days his lips turned faintly blue not always, just when he cried hard or fed for too long.
Two doctors said wait and watch. His parents couldn’t. Not when their six-month-old weighed less than most three-month-olds. So they kept looking. A family friend referred them to a Pediatric Cardiologist in Mumbai who had handled cases like this before. That’s when they met Dr. Prashant Bobhate at Kokilaben Dhirubhai Ambani Hospital.
Symptoms
- Extreme difficulty completing feeds bottles took over an hour
- No weight gain; weight at 6 months matched a 3-month-old
- Excessive sweating during feeds, even in a cooled room
- Occasional bluish discoloration of lips and fingernails
- Visible breathlessness and fatigue after minimal exertion
Diagnostic Method
A thorough clinical evaluation was done before any imaging:
- Physical Examination: Dr. Bobhate detected a loud heart murmur on auscultation, prompting immediate imaging
- 2D Echocardiography : a non-invasive, painless ultrasound of the heart; confirmed the location and size of the defect; Aarav slept through most of it
- Clinical Assessment of Growth Parameters : weight, feeding pattern, and respiratory rate reviewed against age-standard charts
Disease Diagnosed
Based on the echocardiogram findings, Aarav was diagnosed with a Ventricular Septal Defect (VSD) a 10mm hole between the two lower pumping chambers of the heart. Oxygenated blood was leaking back into the lungs instead of circulating to the body. The heart compensated by overworking, which explained the feeding exhaustion, sweating, and poor weight gain. Left untreated, a defect this size carries the risk of permanent lung damage over time.
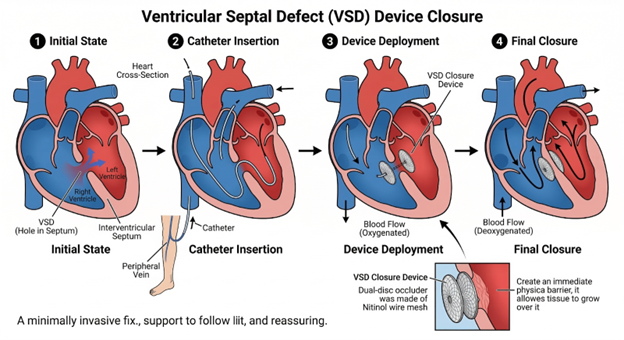
Treatment Plan
After reviewing the echocardiogram and Aarav’s overall condition, Dr. Prashant Bobhate recommended transcatheter device closure a minimally invasive procedure that seals the VSD without opening the chest.
Why Device Closure Was the Right Choice
- The 10mm defect was anatomically suited for catheter-based closure, avoiding the risks of open-heart surgery in a 6-month-old
- A thin flexible tube was inserted through a small vein in Aarav’s leg and guided to the heart under imaging
- A custom closure device was deployed directly over the hole, acting as a permanent plug
- No chest incision. No heart-lung bypass machine. No large scar
- Total procedure time: approximately 90 minutes
- Device closure at this age prevents progressive lung damage that can develop if a large VSD is left untreated beyond infancy
“Device closure has changed how we approach VSDs in infants. When the anatomy allows it, we can fix the heart through a vein in the leg. The child goes home the next morning. That’s the outcome every parent deserves.” — Dr. Prashant Bobhate, Pediatric Cardiologist, Kokilaben Hospital Mumbai
Post-Procedure Guidelines
To support safe recovery and device integration, Aarav’s parents were advised to follow these steps:
- Avoid bathing the leg entry site for 48 hours; keep it dry and clean
- No strenuous handling or rough play for two weeks
- Complete the prescribed antiplatelet medication course as directed
- Watch for fever, unusual irritability, or any swelling near the catheter site
- Attend follow-up echocardiograms at one month and three months post-procedure
Outcome
Recovery was fast. Faster than his parents expected.
Within the first week, Aarav finished his bottles without stopping. No more sweating through his clothes. No more hour-long feeding sessions. He slept through the night.
At the one-month follow-up, the echo confirmed the device was seated perfectly. No residual leak. Heart functions fully normal.
By three months, he had gained two kilograms. His cheeks filled out. He started crawling.
Today, Aarav is a healthy, active toddler. Loud. Curious. Getting into everything. Nothing about him suggests he once had a heart defect.
Long-Term Expectations
Over the next 12 months, the closure device will become fully integrated into the heart wall as natural tissue grows over it. With no residual defect and normal cardiac function confirmed, Aarav is not expected to require any further cardiac intervention. Routine annual follow-ups will continue to monitor growth and heart function through early childhood.
What Aarav's Family Said
“We were told open surgery was the only option. Dr. Bobhate showed us there was another way. Aarav was back home the next day. Within a week he was feeding normally. I still can’t believe how different things are now. We’re just grateful we didn’t wait.” — Priya S., Aarav’s Mother