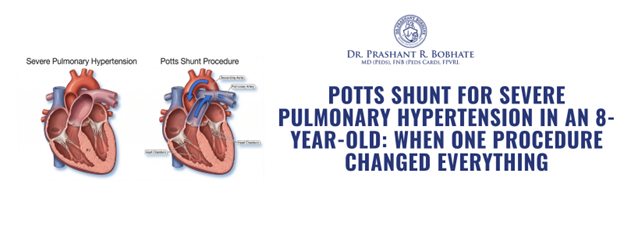
Potts Shunt for Severe Pulmonary Hypertension in an 8-Year-Old: When One Procedure Changed Everything
Patient Profile
Patient Name: Riya M.
Age: 8 years
Gender: Female
Location: Pune, Maharashtra
Patient Background
Riya used to run. Not anymore.
By the time she turned seven, climbing one flight of stairs left her breathless. She’d stop midway, hold the railing, wait. Her classmates ran around at recess. She sat and watched. Her parents assumed it was anaemia. Maybe low fitness. Something simple.
It wasn’t simple.
Over eight months, three hospitals and four opinions later, Riya was diagnosed with severe Pulmonary Arterial Hypertension — dangerously high pressure in the arteries supplying her lungs. Her right heart was failing under the strain. She was on three medications. None of them were working well enough.
Her parents were told she might need a lung transplant. They weren’t ready to accept that. A pulmonologist in Pune referred them to a Heart Specialist for Children in Mumbai who had done this procedure before — more times than anyone else in India. That doctor was Dr. Prashant Bobhate at Kokilaben Dhirubhai Ambani Hospital.
Symptoms
- Severe breathlessness on minimal exertion — couldn’t climb stairs without stopping
- Extreme fatigue; slept far more than a child her age should
- Frequent fainting spells, especially during any physical activity
- Swelling in both legs by evening
- Bluish discolouration of lips during exertion
- Near-complete inability to participate in normal childhood activity
Diagnostic Method
A full cardiac and pulmonary workup was carried out before any intervention decision was made:
- 2D and 3D Echocardiography — confirmed severely elevated right heart pressures and right ventricular dysfunction
- Cardiac Catheterization — direct measurement of pulmonary artery pressure; confirmed suprasystemic pulmonary hypertension (lung pressures exceeding body pressures)
- CT Pulmonary Angiography — ruled out blood clots; assessed pulmonary vascular anatomy
- Six-Minute Walk Test — Riya could barely complete 180 metres; well below normal for her age
- Vasoreactivity Testing — confirmed non-response to conventional vasodilators, ruling out simpler medical management
Disease Diagnosed
Riya was confirmed to have end-stage Pulmonary Arterial Hypertension — Group 1 classification, with suprasystemic pressures and right ventricular failure. Her pulmonary artery pressure exceeded her systemic blood pressure. The right side of her heart was pumping against a wall it couldn’t overcome.
At this severity, standard medications manage symptoms but cannot reverse the haemodynamic damage. Without a structural intervention, the trajectory in cases like Riya’s is predictable and grim. A lung transplant was discussed. But her anatomy and age made her a candidate for something else first.
Treatment Plan
After reviewing all investigations and presenting Riya’s case at a multidisciplinary team meeting, Dr. Prashant Bobhate recommended a Potts Shunt — a surgical connection created between the left pulmonary artery and the descending aorta, designed specifically for children with end-stage pulmonary hypertension.
Why the Potts Shunt Was Chosen
- Riya’s pulmonary pressures had crossed systemic levels — a point where the right heart cannot sustain itself without pressure relief
- The Potts Shunt creates a controlled bypass that offloads the failing right ventricle by allowing excess pressure to vent directly into the body circulation
- This decompresses the right heart, reduces its workload, and allows it to recover function over time
- Unlike a lung transplant, this procedure does not remove the option of transplant later if needed — it buys time and improves quality of life while the heart stabilises
- Bobhate’s team at KDAH has performed 19 Potts Shunt procedures with a success rate exceeding 80% — the highest single-centre experience for this procedure in India
- Post-procedure, most patients are able to resume daily activities on minimal medications
The procedure was performed under general anaesthesia. A connection was created between the left pulmonary artery and the descending aorta using a surgical graft. The right heart now had a release valve. Pressure on the lungs dropped. The heart could breathe again.
Doctor’s Quote: “The Potts Shunt is not a cure. But for children with suprasystemic pulmonary hypertension, it is often the difference between a life spent in a hospital bed and a life actually lived. Riya deserved that chance — and her anatomy gave us the window to take it.” — Dr. Prashant Bobhate, Pulmonary Hypertension Specialist in Mumbai, Kokilaben Hospital
Post-Procedure Guidelines
Recovery required careful monitoring and a structured protocol:
- ICU stay for 48–72 hours post-procedure for haemodynamic monitoring
- Gradual weaning of IV medications as pulmonary pressures stabilised
- Strict activity restriction for 6 weeks — no running, no exertion, no climbing
- Anticoagulation therapy continued as prescribed to protect the shunt
- Pulmonary vasodilator medications continued at adjusted doses
- Follow-up echocardiograms and catheterisation scheduled at 3 months and 6 months post-procedure
- Cardiopulmonary rehabilitation started at week 8 under supervised guidance
Outcome
Three weeks after surgery, Riya walked to the hospital cafeteria with her mother. No stopping. No breathlessness.
Her mother cried in the corridor.
At the three-month follow-up, echocardiography showed significant improvement in right ventricular function. Her six-minute walk distance had increased from 180 metres to 340 metres. She was back in school part-time.
By six months, she was attending full school days. She couldn’t run yet — but she was walking, laughing, eating properly, and sleeping through the night without waking up short of breath.
The lung transplant discussion was quietly set aside.
Long-Term Expectations
The Potts Shunt is not a cure for pulmonary hypertension. Riya will continue on pulmonary vasodilator therapy and require regular cardiac follow-up throughout childhood and adolescence. With right ventricular function now recovering and functional capacity improving month on month, the goal is a stable, active life on manageable medications. If pressures rise again in future years, the shunt does not foreclose any further treatment options including transplantation.
What Riya's Family Said
“We came to Dr. Bobhate when three hospitals had run out of answers. He didn’t promise miracles. He explained exactly what he was going to do and why. Three months later, my daughter walked into her classroom on her own. That’s all I ever wanted.”
— Meena M., Riya’s Mother, Pune
