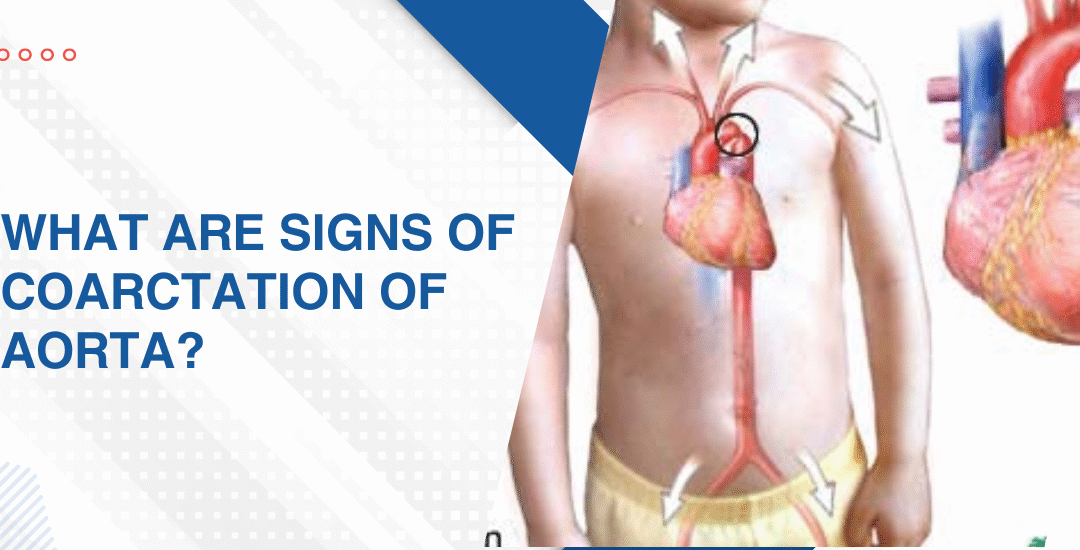
The main signs are usually a big gap between upper and lower body blood pressure, weak or delayed leg pulses next to the arm pulses, babies who struggle during feeds, poor weight gain, tired legs in older kids during play, and in the sharpest cases, a newborn who crashes in the first few weeks of life once the ductus arteriosus starts to close.
“Coarctation is one of those lesions that can sit hidden for years, and the one clinical move that catches it early is simply checking leg pulses and comparing them with the arms, something still missed far more often than it really should be,” says Dr. Prashant Bobhate, Pediatric Cardiologist in Mumbai, India.
What Are the Common Signs of Coarctation of Aorta in Children?
Coarctation doesn’t show up the same way at every age. What you’d spot in a crashing newborn looks nothing like what you’d pick up in a healthy-looking ten-year-old with just a murmur on routine screening.
- Weak or delayed femoral pulses: Leg pulses feeling noticeably softer than the arm pulses, or arriving a beat late, are usually the first real clue on examination.
- Arm pressure high, leg pressure low: A gap of more than 20 mmHg between upper and lower limb pressures is a strong red flag for narrowing somewhere along the aortic arch.
- Breathlessness and poor feeding in infants: Babies tire out halfway through a feed, sweat on the forehead, and gain weight slowly in a way that just doesn’t quite add up on routine paediatric review.
- Leg fatigue or cramping during play: Older kids complain of tired legs, cramps during sport or running, or a strange heaviness that eases the moment they stop, often brushed off as plain unfitness for years.
Any child showing these features really deserves a proper congenital heart disease workup, because coarctation picked up early is so much easier to manage than one found after years of quiet pressure overload on the heart.
How Do Doctors Diagnose and Confirm Coarctation of Aorta?
Clinical findings raise the suspicion. Confirmation, though, always comes down to imaging, and this is really where early diagnosis quietly separates from late diagnosis when you look at long-term outcomes.
- Four-limb blood pressure measurement: Measuring pressure in both arms and both legs is the single most useful bedside test, and a real gap between upper and lower limb pressure is practically diagnostic on its own.
- Echocardiography: A 2D echo usually shows the coarctation site, gives the pressure gradient across it, and tells the clinician how well the left ventricle is coping with the extra load.
- CT or MR angiography: Cross-sectional imaging comes in when the echo isn’t clear, especially in older children, adolescents and young adults where the arch can’t always be seen properly on echo alone.
- Pulse oximetry screening in newborns: Differential saturations between the right arm and the legs can flag critical coarctation even before symptoms start, which is why newborn pulse oximetry matters so much.
Parents wanting a broader read on how critical heart lesions tend to surface in the first days of life can take a look at our piece on signs of a heart problem in a newborn baby, because spotting the pattern early really does change how much room there is to plan the next steps.
Why Choose Dr. Prashant Bobhate for Coarctation of Aorta Evaluation in Mumbai?
Diagnosing coarctation comes down to putting the clinical findings, blood pressure gap and imaging into one clean picture, and then making an honest call on whether this child needs catheter-based intervention, surgical repair or just careful follow-up, rather than drifting between opinions for months. Dr. Prashant Bobhate has spent over 12 years managing congenital aortic lesions across every age group, from critical neonatal presentations right through to adult patients with late-diagnosed coarctation, at the Children’s Heart Centre, Kokilaben Dhirubhai Ambani Hospital.
Schedule a consultation to understand what your child’s findings actually mean, and what the right next step looks like from here.
FAQs
Can coarctation of aorta be missed in a routine check-up?
It really can, because unless the clinician actively checks and compares leg pulses with arm pulses, a child with mild coarctation may go years without any obvious clue pointing toward the diagnosis.
Is coarctation of aorta dangerous if left untreated?
Untreated coarctation leads to long-standing high blood pressure in the upper body, left ventricular strain, and a higher risk of heart failure, stroke and aortic complications later in life, which is why early correction genuinely changes the outlook.
At what age is coarctation usually diagnosed?
Critical coarctation typically turns up in the first weeks of life as the ductus closes, while milder forms may not get picked up until childhood, adolescence, or even adulthood when an incidental finding of high blood pressure triggers the workup.
Is surgery the only treatment for coarctation of aorta?
Surgery is one option, but balloon angioplasty with or without stenting has become a well-established alternative in many children and adults, and the choice really depends on the age, anatomy and severity of the narrowing.
References:
- Coarctation of the Aorta, MedlinePlus, U.S. National Library of Medicine — https://medlineplus.gov/ency/article/000191.htm
- Coarctation of the Aorta, American Heart Association — https://www.heart.org/en/health-topics/congenital-heart-defects/about-congenital-heart-defects/coarctation-of-the-aorta-coa